Basic Planning for Quality
QP-7: Formulating a Total Quality Control Strategy
Total Quality Control Strategies optimize your management of the tests and methods in your laboratory. Learn how to distribute your scarce laboratory resources in this lesson.
Note: This material is covered in the Basic Planning for Quality manual. Updated coverage of these topics can be found in Assuring the Right Quality Right, as well as the Management and Design of Analytical Quality Systems online course.- Review of CLIA regulations
- General TQC guidelines
- Step-by-step TQC guidelines
- HI-Ped strategy
- MOD-Ped and LO-Ped TQC strategies
- Additional steps for LO-Ped TQC strategy
- Cost of quality control vs quality improvement
- References
Optimal management of analytical quality depends on individualizing the QC procedures for each test and method in the laboratory. The quality-planning process provides the methodology for (a) setting method performance specifications that are appropriate for the analytical or clinical quality required for a test and (b) selecting statistical QC procedures appropriate for the actual imprecision and inaccuracy observed for methods in routine operation in a laboratory. Ideally, the QC procedure should provide at least a 90% chance of rejecting an analytical run having medically important errors. At the same time, the QC procedure should have less than a 5% chance of falsely rejecting a run that contains only the random errors due to the inherent (stable) imprecision of the method. And, for practicality and low cost, the QC procedure should require only 2 to 6 control measurements per run - the lower the better.
Review of CLIA regulations
US government regulations (CLIA-88) define a set of standards for quality control that include method performance specifications, statistical quality control, preventive maintenance, instrument function checks, and method performance tests [1,2]. These CLIA rules may be viewed as separate requirements for individual components of Quality Control (QC), or as a requirement for developing a Total Quality Control (TQC) strategy that incorporates these components in a manner appropriate for controlling individual testing processes. The latter view would seem to be more desirable for assuring the quality of laboratory testing because of the need to individualize the QC designs for the many different analytical methods for performing those tests.
The responsibility for establishing a TQC strategy initially belongs to the manufacturers of medical testing systems, devices, or kits. When a manufacturer's QC instructions have by cleared by FDA as meeting CLIA requirements for quality control, the CLIA rules require that a laboratory does the following:
"demonstrate that, prior to reporting patient test results, it can obtain the performance specifications for accuracy, precision, and reportable range of patient test results, comparable to those established by the manufacturer [2, p. 5230, par. 493.1213(b)(1)],
"perform maintenance as defined by the manufacturer and with at least the frequency specified by the manufacturer," [2, p. 5231, par. 493.1215(a)(i)],
"perform function checks as defined by the manufacturer and with at least the frequency specified by the manufacturer" [2, p. 5231, par. 493.1215(b)(i)],
"follow the manufacturer's instructions for calibration and calibration verification procedures using calibration materials specified by the manufacturer" [2, p. 5231, par. 493.1217(a)], and
"follow the manufacturer's instructions for control procedures" [2, p. 5232, par. 493.1218(a)].
For a test method whose QC instructions have not been cleared by the FDA, the laboratory itself assumes responsibility for formulating an appropriate strategy for quality control that includes these same components. Note that as of the year 2000, a QC clearance process has NOT yet been implemented in accordance with the CLIA regulations, thus the laboratory is primarily responsible for selecting appropriate QC procedures and for implementing appropriate TQC strategies.
General TQC Guidelines
The starting point for formulating a TQC strategy is the quality-planning process and the error detection available from the selected statistical QC procedure. Testing processes will be classified into one of three categories: high error detection when a QC procedure can be selected from an OPSpecs chart with 90% AQA; moderate error detection when a QC procedure is selected from an OPSpecs chart with 50% AQA; low error detection when 50% AQA is not obtainable, in which case a maximum QC procedure should be defined as the default selection. The recommendations for maximum QC selections here are to use a multirule procedure such as 13s/22s/R4s/41s/8x with the maximum of N=4 (for 2 control materials) and 13s/2of32s/R4s/31s/6x with N=6 (for 3 control materials).
 The general TQC strategies for these three classes are shown in the accompanying table, where SQC refers to statistical QC, Other QC includes preventive maintenance (PM), instrument function checks (FC), performance validation tests (PV), and patient data quality control (PD). QI means quality improvement and refers primarily to improving the precision, accuracy, and stability of the measurement procedure.
The general TQC strategies for these three classes are shown in the accompanying table, where SQC refers to statistical QC, Other QC includes preventive maintenance (PM), instrument function checks (FC), performance validation tests (PV), and patient data quality control (PD). QI means quality improvement and refers primarily to improving the precision, accuracy, and stability of the measurement procedure.
- HI-Ped strategy. When SQC is able to provide high error detection, then the TQC strategy is to depend primarily on SQC and perform the minimum requirements for other QC components.
- MOD-Ped strategy. When SQC provides moderate error detection, the TQC strategy is to balance the emphasis on SQC, Other QC, and QI.
- LOW-Ped strategy. When SQC provides low error detection, the TQC strategy cannot rely on SQC, but must emphasize Other QC and QI.
Step-by-step guidelines
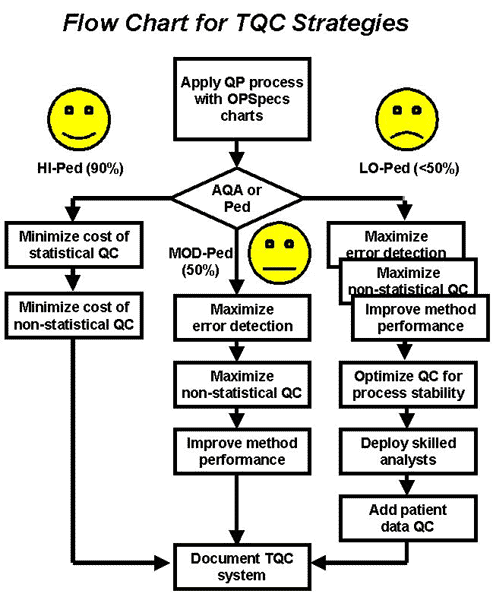
The flowchart shows a more detailed process for developing a TQC strategy for an individual method. When SQC provides high error detection (90% AQA), the emphasis is on minimizing the costs of statistical and non-statistical QC. When SQC provides moderate error detection (at least 50% AQA), then the emphasis is on maximizing statistical and non-statistical components, as well as improving measurement performance. If SQC provide low error detection (less than 50% AQA), the efforts also include optimizing QC for process stability, improving the skills of the analysts, and adding patient data QC. In all cases, the final step is to document the QC system.
HI-Ped Strategy
- Minimize the cost of statistical QC. Use as few control measurements as needed. Reduce N to a minimum of 2 whenever possible. Use single-rule rather than multi-rule procedures. Use control limits as wide as 3.5s when possible to minimize false rejections. Aim for 1% or lower false rejection. Increase run length to maximize test yield, i.e., the ratio of patient samples to control and calibration samples.
- Minimize cost of non-statistical QC. Recognize the limitations of control materials and their matrices when minimizing non-statistical QC. Weigh the clinical needs and risks carefully. Then identify the minimum frequency of system function checks, performance validation tests, and preventive maintenance, as required by regulations, manufacturer's instructions, and good laboratory practice.
- Document the TQC strategy. The last step for any of the TQC strategies is documentation, including the QC acceptability criteria (control rules, N) for assessing the control status of an analytical run. Document the expected rejection characteristics of the statistical QC procedure. Establish the schedule for performing non-statistical QC checks and document the procedures for performing those checks.
MOD-Ped and LO-Ped Strategies
- Maximize error detection. Increase N from a minimum of 2 up to at least 4 control measurements per run when using two control materials and increase N from 3 to 6 when using three control materials. Increase run length as a way of increasing N, being careful to satisfy the turnaround time requirements for the test. Narrow the control limits and tolerate higher false rejections, up to 6-7% for the N=6 procedures. Change from single-rule to multirule QC procedures. Use look-back rules to effectively increase N by inspecting control data from the previous run. Implement multi-stage QC procedures that have startup designs with higher N's and/or more sensitive control rules to maximize error detection, then switch to a monitor design having lower N and/or less sensitive control rules that minimize false rejections. Switch back and forth between the startup and monitor designs as necessary.
- Maximize non-statistical QC. Perform preventive maintenance, calibration, instrument checks, and performance verification tests that are required by CLIA, recommended by the manufacturer, and appropriate for the susceptibility of the method and the clinical application of the test. Adopt a more aggressive schedule to minimize problems.
- Improve method performance. Reduce analytical bias by selecting appropriate standards, calibrating properly, and by selecting proper comparison groups in proficiency testing surveys. Reduce imprecision by identifying and minimizing the major component of variance, standardizing operator techniques, and mechanizing manual steps in the process. Reduce frequency of errors by identifying and eliminating sources of problems, increasing the preventive maintenance schedule, increasing function checks and performance verification tests, reducing operator variables, and increasing operating training and expertise. When necessary, change measurement procedures or analytic systems to obtain better accuracy, precision, and stability.
Additional steps for LO-Ped strategy
- Optimize QC for process stability. Document the frequency of errors by careful study of the analytical process. In general, a 50% error detection rate will be satisfactory for stable processes that have <2% frequency of errors and even a 25% detection rate may be sufficient for extremely stable processes that have <1% frequency of errors.
- Deploy skilled analysts. Assign highly skilled analysts to testing processes that are problematic and difficult to control. Provide thorough in-service training. Increase technical skills and experience. Improve problem-solving capabilities. Improve statistical skills for method validation and quality control. Reduce the rotation schedule for personnel to maintain operator experience and continuity.
- Add patient data QC. Perform between system comparisons on patient samples. Check patient data with consistency algorithms, such as delta checks, anion gap, etc. Utilize population statistics, such as mean of normals, Bull's algorithm, etc. Perform clinical correlations to check test results with patient diagnosis and condition.
Cost of quality control vs cost of quality improvement
 The costs of quality control are ongoing and never-ending, month after month, year after year. The accompanying figure illustrates the relative costs for different TQC strategies.
The costs of quality control are ongoing and never-ending, month after month, year after year. The accompanying figure illustrates the relative costs for different TQC strategies.
- HI-Ped TQC costs. When 90% detection of medically important errors can be achieved with statistical QC, cost of ongoing quality management is lowest. The better the analytical performance, the lower number of control measurements needed, the wider the control limits, the lower the false rejection rate, and the less non-statistical QC is needed. This demonstrates Deming's principle that improved quality leads to lower costs.
- MOD-Ped TQC costs. When moderate error detection is achieved - greater than 50% detection of medically important errors, all the costs go up, including the cost of statistical QC. There is a need for more control measurements, more preventive maintenance, more frequent instrument checks, etc., which means more time and effort by laboratory personnel.
- LO-Ped TQC costs. When error detection is low - less than 50% detection of medically important errors, costs become even greater. There is a need for more training, more operator experience, and more review and correlation of patient data.
At some point, the costs for MOD-Ped TQC and LO-Ped TQC should justify efforts to improve the performance of an analytical method. Begin your quality improvement efforts by reducing the inaccuracy or bias of the method. Next try to reduce the imprecision or CV of the method. Try to gain enough improvement to change the TQC strategy, moving from LO-Ped to MOD-Ped to HI-Ped strategies. If this is not successful, consider replacing the method with one that has better analytical performance.
REFERENCES
- Health Care Financing Administration (HCFA) and Public Health Service (PHS), US Dept of Health and Human Services (HHS). Medicare, Medicaid and CLIA Programs. Regulations implementing the Clinical Laboratory Improvement Amendments of 1988 (CLIA) and Clinical Laboratory Improvement Act program fee collection. Fed Regist 1993;58:5215-37.
- U.S. Dept. of Health and Human Services. Medicare, Medicaid, and CLIA Programs: regulations implementing the Clinical Laboratory Improvement Amendments of 1988 (CLIA). Final Rule. Fed Regist 1992;57:7002-186.